
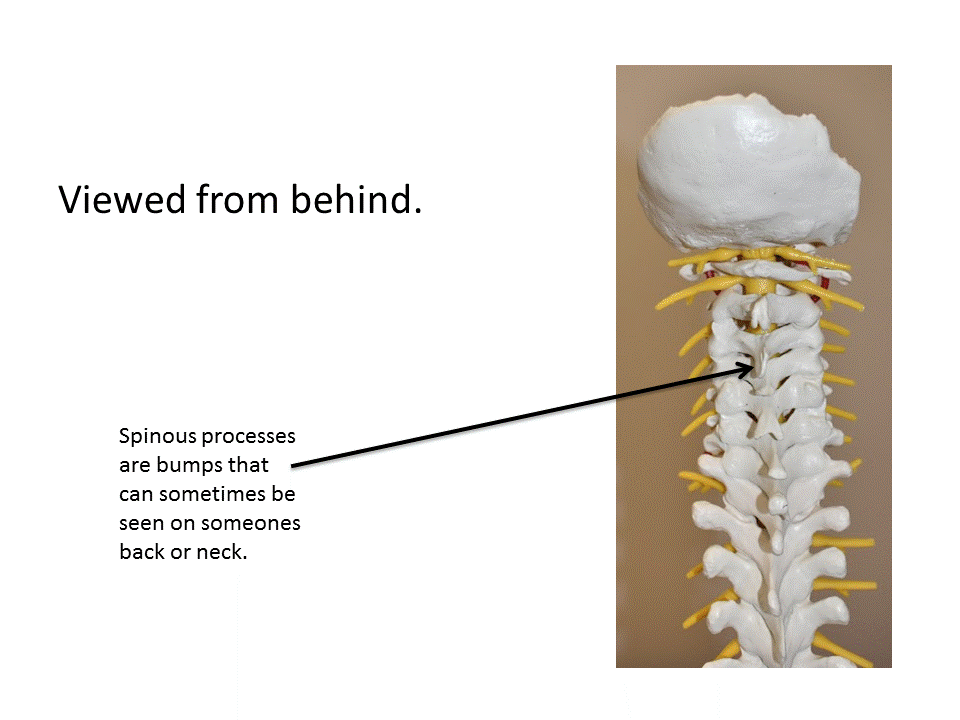
What is cervical myelopathy?
Cervical myelopathy is the medical term used when the spinal cord in the neck is not working normally.
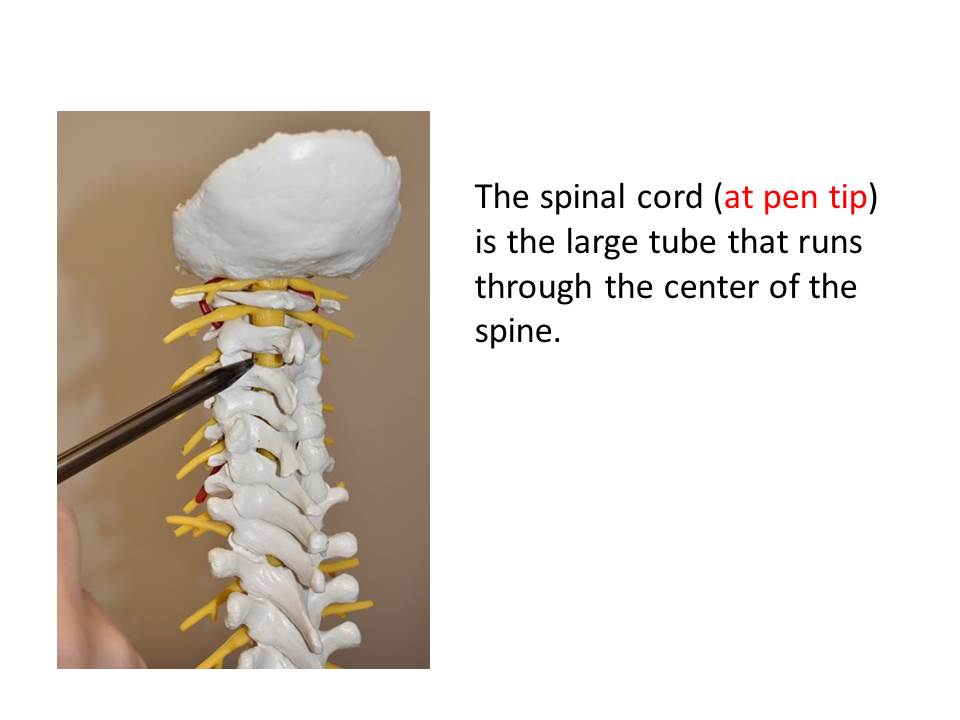
What is the function of the spinal cord?
The spinal cord is a very important neurological structure that connects the brain to the rest of the body. It’s a pathway for all the information signals going into the brain, as well as outgoing commands from the brain to your arms, legs, and organs. This includes sensation (feeling) in the arms and legs which includes sense of touch but also sensation important for balance and coordination. The spinal cord connects the brain to the nerves in your arms and legs which controls movement by your muscles. It also connects the brain to organs (importantly the bowel and bladder).
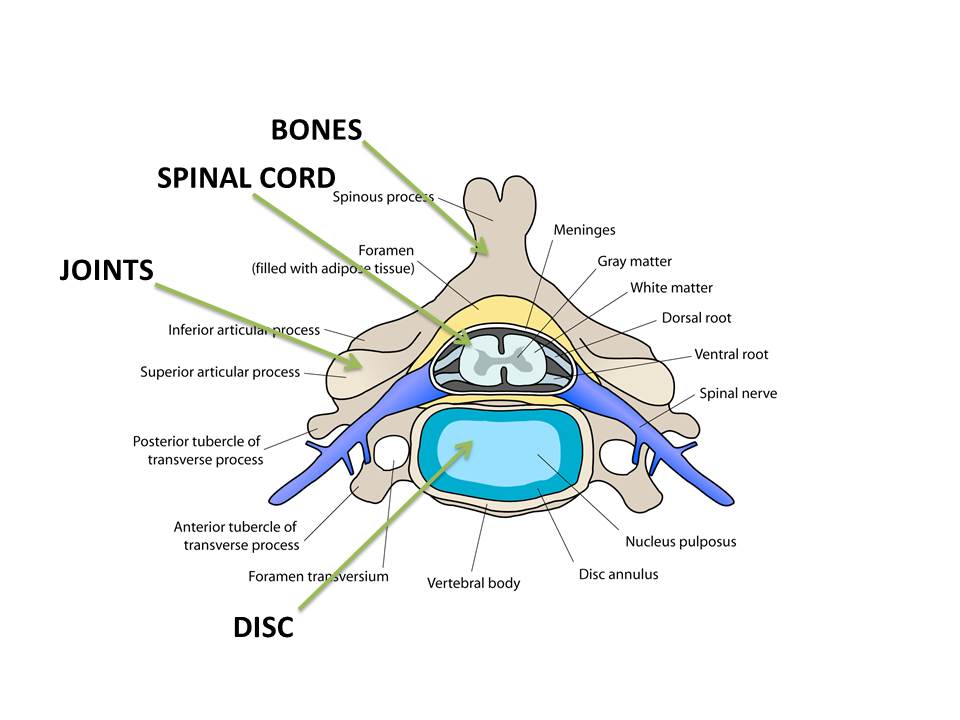
What causes cervical myelopathy?
There are some medical diseases that can affect spinal cord function, but the most common reason is due to compression of the spinal cord inside the spine in the neck. There is a central canal where the spinal cord travels through. When that central passageway is narrowed it is called central spinal stenosis.
This narrowing usually comes about because of a combination of changes to the disc, joints, and ligaments that results in less room for the spinal cord.
Disc herniation: Rubbery discs sit in between each of the vertebrae (spine bones) to add cushion and allow movement. The discs have a tough outer shell and jelly-like center. The discs can break open and bulge out, causing them to press on the spinal cord. (A disc that breaks open and protrudes is called a “herniated disc.”)
Cervical spondylosis: Wear and tear changes in the spine can form bumps called bone spurs which makes the joints in the neck enlarged. This is the same kind of process that happens when we develop osteoarthritis changes in the hand with larger “knobby” knuckles. Ligaments in the front or back of the canal can also thicken with age and leave less room for the spinal cord.
How is cervical myelopathy diagnosed?
Cervical myelopathy is diagnosed based on a combination of your symptoms, physical examination findings, and an MRI.
Symptoms of spinal cord compression are due to interruption of that connection between your brain and your arms and legs. When the sensation pathways are malfunctioning patients experience burning, numbness, and tingling in their hands. This can be quite painly. Most often this is a constant feeling rather than something that comes and goes intermittently. This also affects the use of the hands because of the lack of normal feeling. Coordination is reduced with things like writing, typing, texting, or doing up buttons. Loss of coordination in the legs causes poor balance (not dizziness) that might lead to tripping or falling.
Besides loss of sensation and coordination there are other physical signs that are more specific for a doctor to detect cervical myelopathy. The spinal cord compression affects reflexes in your arms and legs that become very hyperactive as well as tightness in the muscles (spasticity) that your doctor can detect on examination.
On the suspicion or your story and physical exam findings your doctor will order an MRI. An MRI is the best way of getting pictures of your spine and spinal cord to detect this compression.
How is cervical myelopathy treated?
The first thing I tell patients after being diagnosed with cervical myelopathy is to be careful with their neck. This includes avoiding activities that would put them at risk for a head/neck injury. This usually means stopping any sports. I also advise avoiding heavy lifting (your arms dangle off your neck attached almost completely by muscles), avoid chiropractic manipulation, and avoid sustained/awkward neck postures (e.g. fixing the plumbing, looking up for hours while painting the walls).
The definitive treatment for cervical myelopathy is surgery.
What happens if cervical myelopathy is left untreated?
If left untreated 4 things might happen:
- Some people might improve slowly without intervention. This is most hopeful if the spinal cord compression has come acutely from a disc herniation and might resorb by itself.
- Some people will remain stable for periods of time.
- Slow deterioration is possible with some patients with this condition. This could be progressive weakness, poor balance with falls, weakness, hand burning feelings, and loss of bladder control.
- A worst case is sudden spinal cord damage if there is a head/neck injury (usually from a fall). This could cause a sudden paralysis.
What should I do if things are getting worse?
Signs of progression (worsening) include:
- worsening balance (tripping/falling, needing to use cane or walker)
- deteriorating hand function (buttons, typing, texting)
- arm and leg weakness
- bladder urgency leading to loss of control
If this occurs you should contact your doctor to expedite your assessment for surgery. If this happens rapidly (e.g. over the course of a day), you should go to the emergency room for urgent assessment.
What are the consequences of spinal cord compression and how are they treated?
It is better to prevent spinal cord damage than treat the results of it.
Burning pain in the hands is a common consequence of spinal cord compression. Usually treatments for this pain include nerve pain medications (e.g. gabapentin, pregabalin, duloxetine, etc.). These medications are somewhat helpful for pain relief but must be taken every day.
Poor balance (ataxia) if mild can be improved by training your balance under the guidance of a physiotherapist. More severe balance problems require the use of gait aids (e.g. canes, walkers) to reduce the chances of falls or injury.
Bladder changes can occur with spinal cord compression. Usually this is bladder urgency where once someone feels the urge to void they have to go immediately. Sometimes if they can’t get to the bathroom fast enough it might result in a bladder accident (incontinence). There are medicines that can be taken on a daily basis to relax the bladder if this is a problem.
Some patients suffer tight muscles (spasticity) from the spinal cord compression that might interefere with function. If it interferes with function you should be referred to a physiatrist with special training in managing spasticity including medications, injections, and bracing.